

Fudan University Children’s Hospital


 This article introduces a recent study published in the Canadian Journal of Anesthesia titled “Applied forces with direct versus indirect laryngoscopy in neonatal intubation: a randomized crossover mannequin study.”
Approximately 1% of newborns require intubation at birth, and implementing less invasive methods significantly reduces healthcare personnel exposure during neonatal intubation. Previous studies have reported a wide range of intubation success rates among pediatric residents and neonatal fellows (20-70%).
During direct laryngoscopy, the traditional laryngoscope is placed into the mouth and lifted, applying force to the base of the tongue to expose the vocal cords. This maneuver may cause direct trauma to the tissue and lead to adverse reactions. In neonates, the incidence of adverse events during intubation is high, such as esophageal intubation, airway injury, significant bradycardia, and severe intraventricular hemorrhage.
Recent studies indicate that visual laryngoscopy can reduce the occurrence of adverse events during neonatal intubation and improve the success rate for inexperienced healthcare personnel. Visual laryngoscopes allow indirect observation of the larynx using a camera, employing curved blades (Macintosh), straight blades (Miller), or modified blades. Notably, compared to the 15-30 degree view provided by Macintosh or Miller blades, hyperangulated blades can offer a 60-90 degree view of the laryngeal structures, enabling visualization of the glottis without aligning the mouth, pharynx, and larynx. However, since this visual laryngoscope does not allow direct observation of the vocal cords, a stylet should be used to pre-shape the endotracheal tube (ETT) to match the curvature of the blade.
According to an adult mannequin study, visual laryngoscopy improves glottic visualization, applies less force to the upper airway tissues, and reduces workload compared to direct laryngoscopy. We hypothesize that this method may provide similar benefits during neonatal intubation. To investigate this, we compared the oropharyngeal forces and perceived workload during the use of direct laryngoscopy, visual laryngoscopy with a standard blade, and visual laryngoscopy with a hyperangulated blade on a neonatal mannequin.
This is a randomized, controlled, crossover trial using three types of laryngoscopes for intubation in a neonatal mannequin. The trial implemented six sequences, three periods, and three treatment protocols (ABC/BCA/CAB/ACB/BAC/CBA), which were uniform within sequences and periods and balanced regarding first-order carryover effects. The experiment was conducted between January 20-26, 2022, at the University of Padua in Italy, and was deemed a simulation study on a mannequin by the Padua University Ethics Committee (protocol number 0002658), thus not requiring formal ethical approval. Written informed consent was obtained from participants.
Consultants from the tertiary neonatal intensive care unit (NICU) and pediatric intensive care unit (PICU), pediatric residents, anesthesia consultants, and anesthesia residents participated in the study. Exclusion criteria included refusal to participate.
All participants were randomly assigned to one of the six sequences in a 1:1:1:1:1:1 ratio using a computer-generated random allocation list, and the researchers placed the allocation results in sealed opaque envelopes marked with sequential numbers.
Participants in the ABC group were first assigned to intubate using direct laryngoscopy (A), followed by visual laryngoscopy with a standard blade (B), and then visual laryngoscopy with a hyperangulated blade (C). Participants in different groups were assigned to intubate in different orders (BCA/CAB/ACB/BAC/CBA). The experiment included a four-hour washout period.
Before the simulation began, an expert in visual laryngoscopy demonstrated the intubation technique using a Miller blade and a hyperangulated blade on the neonatal mannequin to each participant, followed by demonstrating the intubation technique using a direct laryngoscope with a Miller blade. Each participant was required to practice with all devices on the mannequin before recording the laryngoscopy trial.
During the simulation, participants were required to intubate a term neonatal mannequin (Annie) using three different laryngoscopes: a standard direct laryngoscope with a #1 Miller blade, a visual laryngoscope with a Miller blade, and a visual laryngoscope with a hyperangulated blade. Each intubation attempt used a 3mm ETT, with a stylet inserted into the ETT. During intubation with the hyperangulated visual laryngoscope, a pre-shaped stylet was used.
During each intubation attempt, the researchers recorded the intubation time and the number of attempts. If the ETT was not placed in the trachea or the attempt lasted more than 60 seconds, the intubation attempt was considered a failure. This interval was chosen considering the varying intubation experience of our participants.
In each procedure, three force sensors (FlexiForce A301; Tekscan, Inc., Norwood, MA, USA) were affixed with double-sided tape at three different locations on each blade to measure the force. One sensor (epiglottis sensor) was placed on the distal surface of the blade, corresponding to the area that contacts the epiglottis during intubation, and the other two sensors (palate sensors) were placed on the proximal surface of the blade, corresponding to the areas that contact the upper gums and hard palate. The entire blade surface was then covered with a heat-shrink tube, concealing the sensors from the participants and protecting them during the experiment. Each force sensor had a sensing area of 9.53 mm in diameter, a thickness of 0.203 mm, a response time of less than 5 seconds, a linear error of ± 3%, and a pressure range of 0-111 N. The output signals from the sensors were adjusted and amplified using electronic components recommended in the sensor data sheet and were collected via an Arduino Uno board. Data from each sensor were filtered using a moving average filter of 10 samples to remove some noise and were saved in text files. A calibration curve for each laryngoscope sensor was inferred from bench tests and integrated into the LabVIEW script. A graphical user interface was implemented for real-time debugging and visualization of the collected data, as shown in the electronic supplementary material (ESM) eFig. Data collection started when the laryngoscope was placed in the mouth and ended when it was removed, ensuring sufficient sampling of the sensor signals using the selected Arduino board and its interface with LabVIEW software.
This article introduces a recent study published in the Canadian Journal of Anesthesia titled “Applied forces with direct versus indirect laryngoscopy in neonatal intubation: a randomized crossover mannequin study.”
Approximately 1% of newborns require intubation at birth, and implementing less invasive methods significantly reduces healthcare personnel exposure during neonatal intubation. Previous studies have reported a wide range of intubation success rates among pediatric residents and neonatal fellows (20-70%).
During direct laryngoscopy, the traditional laryngoscope is placed into the mouth and lifted, applying force to the base of the tongue to expose the vocal cords. This maneuver may cause direct trauma to the tissue and lead to adverse reactions. In neonates, the incidence of adverse events during intubation is high, such as esophageal intubation, airway injury, significant bradycardia, and severe intraventricular hemorrhage.
Recent studies indicate that visual laryngoscopy can reduce the occurrence of adverse events during neonatal intubation and improve the success rate for inexperienced healthcare personnel. Visual laryngoscopes allow indirect observation of the larynx using a camera, employing curved blades (Macintosh), straight blades (Miller), or modified blades. Notably, compared to the 15-30 degree view provided by Macintosh or Miller blades, hyperangulated blades can offer a 60-90 degree view of the laryngeal structures, enabling visualization of the glottis without aligning the mouth, pharynx, and larynx. However, since this visual laryngoscope does not allow direct observation of the vocal cords, a stylet should be used to pre-shape the endotracheal tube (ETT) to match the curvature of the blade.
According to an adult mannequin study, visual laryngoscopy improves glottic visualization, applies less force to the upper airway tissues, and reduces workload compared to direct laryngoscopy. We hypothesize that this method may provide similar benefits during neonatal intubation. To investigate this, we compared the oropharyngeal forces and perceived workload during the use of direct laryngoscopy, visual laryngoscopy with a standard blade, and visual laryngoscopy with a hyperangulated blade on a neonatal mannequin.
This is a randomized, controlled, crossover trial using three types of laryngoscopes for intubation in a neonatal mannequin. The trial implemented six sequences, three periods, and three treatment protocols (ABC/BCA/CAB/ACB/BAC/CBA), which were uniform within sequences and periods and balanced regarding first-order carryover effects. The experiment was conducted between January 20-26, 2022, at the University of Padua in Italy, and was deemed a simulation study on a mannequin by the Padua University Ethics Committee (protocol number 0002658), thus not requiring formal ethical approval. Written informed consent was obtained from participants.
Consultants from the tertiary neonatal intensive care unit (NICU) and pediatric intensive care unit (PICU), pediatric residents, anesthesia consultants, and anesthesia residents participated in the study. Exclusion criteria included refusal to participate.
All participants were randomly assigned to one of the six sequences in a 1:1:1:1:1:1 ratio using a computer-generated random allocation list, and the researchers placed the allocation results in sealed opaque envelopes marked with sequential numbers.
Participants in the ABC group were first assigned to intubate using direct laryngoscopy (A), followed by visual laryngoscopy with a standard blade (B), and then visual laryngoscopy with a hyperangulated blade (C). Participants in different groups were assigned to intubate in different orders (BCA/CAB/ACB/BAC/CBA). The experiment included a four-hour washout period.
Before the simulation began, an expert in visual laryngoscopy demonstrated the intubation technique using a Miller blade and a hyperangulated blade on the neonatal mannequin to each participant, followed by demonstrating the intubation technique using a direct laryngoscope with a Miller blade. Each participant was required to practice with all devices on the mannequin before recording the laryngoscopy trial.
During the simulation, participants were required to intubate a term neonatal mannequin (Annie) using three different laryngoscopes: a standard direct laryngoscope with a #1 Miller blade, a visual laryngoscope with a Miller blade, and a visual laryngoscope with a hyperangulated blade. Each intubation attempt used a 3mm ETT, with a stylet inserted into the ETT. During intubation with the hyperangulated visual laryngoscope, a pre-shaped stylet was used.
During each intubation attempt, the researchers recorded the intubation time and the number of attempts. If the ETT was not placed in the trachea or the attempt lasted more than 60 seconds, the intubation attempt was considered a failure. This interval was chosen considering the varying intubation experience of our participants.
In each procedure, three force sensors (FlexiForce A301; Tekscan, Inc., Norwood, MA, USA) were affixed with double-sided tape at three different locations on each blade to measure the force. One sensor (epiglottis sensor) was placed on the distal surface of the blade, corresponding to the area that contacts the epiglottis during intubation, and the other two sensors (palate sensors) were placed on the proximal surface of the blade, corresponding to the areas that contact the upper gums and hard palate. The entire blade surface was then covered with a heat-shrink tube, concealing the sensors from the participants and protecting them during the experiment. Each force sensor had a sensing area of 9.53 mm in diameter, a thickness of 0.203 mm, a response time of less than 5 seconds, a linear error of ± 3%, and a pressure range of 0-111 N. The output signals from the sensors were adjusted and amplified using electronic components recommended in the sensor data sheet and were collected via an Arduino Uno board. Data from each sensor were filtered using a moving average filter of 10 samples to remove some noise and were saved in text files. A calibration curve for each laryngoscope sensor was inferred from bench tests and integrated into the LabVIEW script. A graphical user interface was implemented for real-time debugging and visualization of the collected data, as shown in the electronic supplementary material (ESM) eFig. Data collection started when the laryngoscope was placed in the mouth and ended when it was removed, ensuring sufficient sampling of the sensor signals using the selected Arduino board and its interface with LabVIEW software.

The primary outcome measure was the maximum peak force during intubation (the maximum force recorded, expressed in Newtons [N]), analyzed using MATLAB software. Data unrelated to the intubation phase (records before insertion and after removal of the laryngoscope from the mouth) were discarded, and the primary outcome measure was derived from the analysis of the relative maximum values of valid data. The relative maximum was determined as the value where the sign of the derivative changed and was organized into a vector. The maximum and average peak forces were then calculated from the vector.
The secondary outcome measures included recording the average peak force during intubation (the average of all peak forces), the time required for intubation, and the subjective workload. The time required for intubation was defined as the period from placing the laryngoscope in the mouth to the time the ETT passed through the vocal cords and the stylet was removed. The subjective workload for each laryngoscope was assessed using the NASA Task Load Index (NASA TLX; NASA Ames Research Center, Mountain View, CA, USA) protocol, which is based on six factors (mental demand, physical demand, time demand, performance, effort, and frustration level). The calculation for NASA TLX is as follows: 1) before the simulation, participants assigned weights to the six factors; 2) at the end of each intubation, participants rated the six factors on a visual rating scale; 3) at the end of the simulation, the weighted sum of the factors was calculated, yielding the NASA TLX. For each participant, assuming that the contribution of the six factors to their workload was similar, we used the same set of weights described in the NASA TLX manual to score the laryngoscopes.
All data were collected by observers not involved in the simulation, recorded on data sheets designed for the study, and stored on a password-protected computer.
The characteristics of the interventions did not allow blinding of participants and outcome assessors; however, the statistician analyzing the data was unaware of the experimental assignments.
Since we could not predict the magnitude of the differences in forces applied using the laryngoscopes, a formal sample size calculation could not be performed during the study planning; thus, this trial chose a sample size of 30 participants.
In the force analysis, the relevant indicators for calculating the maximum peak force and average peak force were the 50th percentile (median) and 10th percentile, and the median and 10th percentile of the paired differences between the two devices were compared. We chose the top 10 percentile differences in force to evaluate the maximum differences in applied force. Bootstrap confidence intervals (CIs) for percentiles and differences were calculated, with a CI for the difference (excluding 0) indicating statistical significance.
Due to coverage errors in the Bootstrap CI for percentiles with small sample sizes, we used a resampling and replacement method to compute empirical Bootstrap 99% CI, creating 1000 samples equivalent to the original sample size.
Intubation time and NASA TLX scores were analyzed similarly: medians (empirical bootstrap 99% CI) were calculated as relevant indicators, and the median of paired differences between the two devices was compared. Statistical analysis was performed using R 4.1 (R Foundation for Statistical Computing, Vienna, Austria).
This trial included 7 level III NICU and PICU consultants, 15 pediatric residents, 7 anesthesia consultants, and 1 anesthesia resident. Among the participants, 17 had limited experience (fewer than 10 intubations) with direct laryngoscopy, 5 had moderate experience (10-50 intubations), and 8 had extensive experience (more than 50 intubations). Twenty-three participants had limited experience (fewer than 10 intubations) with visual laryngoscopy, 2 had moderate experience (10-50 intubations), and 5 had extensive experience (more than 50 intubations).
We obtained complete data from all participants using direct laryngoscopy (A), visual laryngoscopy with a standard blade (B), and visual laryngoscopy with a hyperangulated blade (C). All participants performed the assigned procedures, and there were no losses to follow-up.
Table 1 shows the median and top 10 percentile values of the maximum peak force and average peak force recorded by the epiglottis sensor. Compared to visual laryngoscopy with a standard blade, the median difference for direct laryngoscopy was greater than 0 (maximum peak, 3.2 N; 99% CI, 1.2 -6.1; average peak, 3.1 N; 99% CI, 0.9-5.9), as well as the top 10 percentile difference (maximum peak, 8.2 N; 99% CI, 6.4 -11.7; average peak, 6.7 N; 99% CI, 5.5 ~ 8.4).
Compared to visual laryngoscopy with a hyperangulated blade, the median difference for direct laryngoscopy was greater than 0 (maximum peak, 5.3 N; 99% CI, 3.9-7.2; average peak, 4.9 N; 99% CI, 3.7-7.0), as well as the top 10 percentile difference (maximum peak, 8.7 N; 99% CI, 5.6-11.1; average peak, 7.3 N; 99% CI, 4.1-8.8).
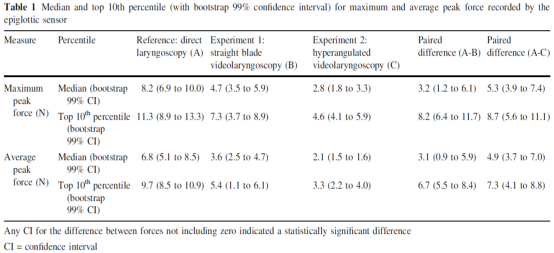
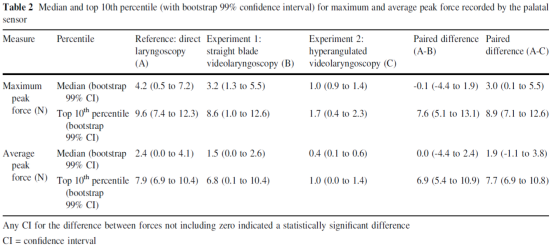
Table 2 shows the median and top 10 percentile values of the maximum peak force and average peak force recorded by the palate sensor. No median difference was found between direct laryngoscopy and visual laryngoscopy with a standard blade (maximum peak, -0.1 N; 99% CI, -4.4 -1.9; average peak, 0.0 N; 99% CI, -4.4-2.4), while the top 10 percentile difference was greater than 0 (maximum peak, 7.6 N; 99% CI, 5.1 -13.1; average peak, 6.9 N; 99% CI, 5.4-10.9).
Compared to visual laryngoscopy with a hyperangulated blade, the median difference for maximum peak force (3.0 N; 99% CI, 0.1-5.5) was greater than 0, but the median difference for average peak force (1.9 N; 99% CI, -1.1-3.8) was not greater than 0, while the top 10 percentile difference was greater than 0 (maximum peak, 8.9 N; 99% CI, 7.1-12.6; average peak, 7.7 N; 99% CI, 6.9-10.8).
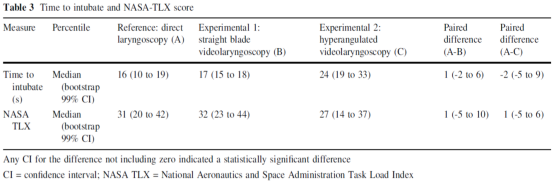
Two participants using direct laryngoscopy, two using visual laryngoscopy with a standard blade, and three using visual laryngoscopy with a hyperangulated blade required more than one attempt. No significant median differences were observed in intubation time or NASA-TLX scores between groups B or C compared to group A (Table 3).
In a neonatal mannequin, the force required for intubation using visual laryngoscopy was less than that using direct laryngoscopy. No detectable differences were found between the two groups in terms of intubation success rate, intubation time, and perceived workload. The reduction in applied force may be an ideal benefit of visual laryngoscopy (i.e., potentially reducing patient harm), but the clinical significance needs to be assessed in future studies.

“Aier Xiaozui” Review
In the neonatal mannequin, the force required for intubation using visual laryngoscopy was less than that using direct laryngoscopy. Additionally, no significant differences were found between the two groups in terms of intubation success rate, intubation time, and subjective workload. The advantages of this study include a crossover design, precise and reliable technical solutions providing objective and reliable force measurements, and the involvement of healthcare personnel with varying levels of experience in using the laryngoscopes. Nevertheless, we should be aware of the limitations of this study. Firstly, the mannequin eliminated anatomical differences between patients; secondly, while literature indicates that the forces used in adult models are very close to those used in humans, the magnitude of the recorded forces may be affected by the low-stress environment of the simulation; thirdly, the findings can only be generalized to healthcare personnel with similar experience. For neonatal and infant intubation, we still recommend using intubation tools that one is familiar with and establishing the airway safely according to the actual situation until new clinical evidence emerges.
Chen Yue
Original Literature:Francesco Cavallin, MSc . Chiara Sala, MD . Sabina Maglio, MSc . Benedetta Bua, MD .Paolo Ernesto Villani, MD . Arianna Menciassi, PhD . Selene Tognarelli, PhD .Daniele Trevisanuto, MD. Applied forces with direct versus indirect laryngoscopy in neonatal intubation: a randomized crossover mannequin study. Can J Anaesth;2023 Feb 14.
doi: 10.1007/s12630-023-02402-9.
Welcome to follow the Gu Ma Jin Zui video account
 Disclaimer: The Gu Ma Jin Zui public account is under Shuyi Hui. The intellectual property rights of the content published by the Gu Ma Jin Zui public account belong to Shuyi Hui and the organizers, original authors, and other related rights holders. Unauthorized reproduction, excerpting, copying, cutting, recording, etc. are prohibited. Authorized use must also indicate the source. Sharing and forwarding are welcome.
Disclaimer: The Gu Ma Jin Zui public account is under Shuyi Hui. The intellectual property rights of the content published by the Gu Ma Jin Zui public account belong to Shuyi Hui and the organizers, original authors, and other related rights holders. Unauthorized reproduction, excerpting, copying, cutting, recording, etc. are prohibited. Authorized use must also indicate the source. Sharing and forwarding are welcome.











 Disclaimer: The Gu Ma Jin Zui public account is under Shuyi Hui. The intellectual property rights of the content published by the Gu Ma Jin Zui public account belong to Shuyi Hui and the organizers, original authors, and other related rights holders. Unauthorized reproduction, excerpting, copying, cutting, recording, etc. are prohibited. Authorized use must also indicate the source. Sharing and forwarding are welcome.
Disclaimer: The Gu Ma Jin Zui public account is under Shuyi Hui. The intellectual property rights of the content published by the Gu Ma Jin Zui public account belong to Shuyi Hui and the organizers, original authors, and other related rights holders. Unauthorized reproduction, excerpting, copying, cutting, recording, etc. are prohibited. Authorized use must also indicate the source. Sharing and forwarding are welcome.